AI for Elderly Dietary Care: A Cyber-Physical System for Nutrition Management
Written by Alva Yeung and Charlie Wu
This article outlines the design and implementation of a cyber-physical system (CPS) that provides nutrition management based on individual elderly patient’s health conditions. The system uses a mobile phone-based app to monitor patient’s state along with reference data from electronic patient record (EPR). The backend CPS provides related nutrition dietary recommendation according to nutrition values that specifically addresses dietary restrictions for various chronic diseases such as hypertension and diabetes. The support system can provide patient with an option of either making self-cooking based on what is currently stored in the fridge with the system generated procedures to follow through or through delivery of ready-to-eat meals.
Artificial intelligence (AI) has been widely used in various sectors of elderly care [1]. AI nutrition management is particularly suited for offering optimal meal based on individual patient’s needs. One of the important features of AI is to provide highly-customized recommendation that caters for the patient’s own circumstances. For example, a diabetes patient that also experiences difficulty with chewing can benefit from a low-sugar nutritious fluid meal composed of appropriate ingredients with a viscosity suitable for safe intake.
The nutrition management CPS can form an integrated part of the broader smart city context in implementing therapeutic lifestyle changes (TLC). TLC includes management of diet, weight and exercise [2]. The urgent need of providing nutritious soft meal is particularly staggering for stroke patients [3]. To support independent living for senior citizens, the system needs to evaluate parameters such as vascular risk factors, cognition and motor abilities to determine the choking risk of eating [4]. The system needs to profile the individual patient’s condition as well as to monitor any subsequent health degradation in addition to learning from the EPR.
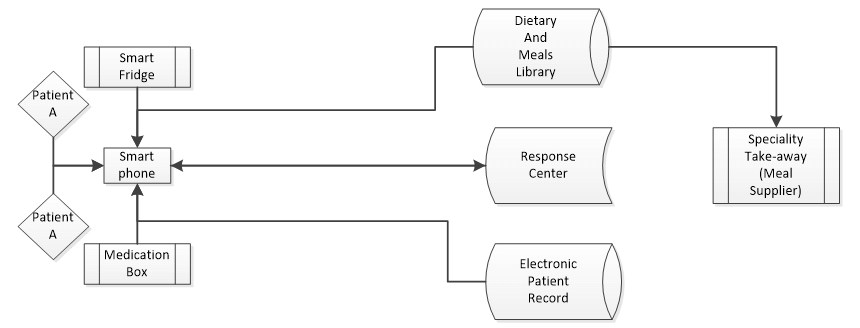
The overall CPS layout is shown in Fig. 1 where the user part is centered upon the user’s smartphone that serves multiple purposes in terms of supporting TLC. At the backend it integrates into the smart city infrastructure and support center. Various entities are interconnected as an internet-of-things (IoT) system with a high degree of service reliability illustrated in [5], all supported across the smart city via a telemedicine network [6]. This particular example supports one elderly couple that share a smartphone, optionally connected to wearable health monitors such as oximeter and glucose monitors.
Figure 1 Nutrition management cyber-physical system
This layout effectively splits between the smart home on the left and the smart city on the right, interconnected by a telemedicine link. The major contributions perceived from the smart city’s perspective is to provide an option for the patients on either to have the customized meals made and delivered or to guide the patient on cooking on one’s own. The patient can obtain all necessary information through the smartphone app. For example, detailed information about how to prepare a soft meal optimized for the patient’s specific conditions is shown in Fig. 2. Therefore, the main sources of revenue would be a user subscription and the sales of both cooking ingredients and commission from meal suppliers. The response center can also generate further income by offering a wide range of add-on assistive healthcare services and solutions [7].

Figure 2 Multi-purpose app for optimizing soft meal
Fig. 2 shows the user interface where the patient can obtain information about state of health, recommended diet and either to access detailed instruction for cooking or to place an online order for the meal to be made and delivered by a specific time. In this particular example, the patient is warned of his blood glucose being on the high side in red, followed by the recommendation of most suitable meal in green with its total amount of calories. Clicking on the picture of the meal will reveal other details like nutrition values and required ingredients currently stored in the fridge. There is also a chart that can be scrolled to display a range of health signs like cholesterol, blood glucose concentration and oxygen saturation. At the bottom of the screen there are two green buttons: left shows detailed cooking instructions and the right button is for the user to order the meal for delivery by a specified time.
This app not only address the specific needs of the patient’s all meals throughout the day but also keeps track of different health signs automatically through an array of health monitoring sensors [8]. It also supports preventive care such as fall detection and will automatically generate an alert when assistance is needed. In addition, the system monitors patient’s daily activities so that meal recommendations can be made with information about the patient’s cholesterol level and heart condition [9]. This can also reduce the risk of developing a range of cardiac diseases such as coronary artery disease (CAD).
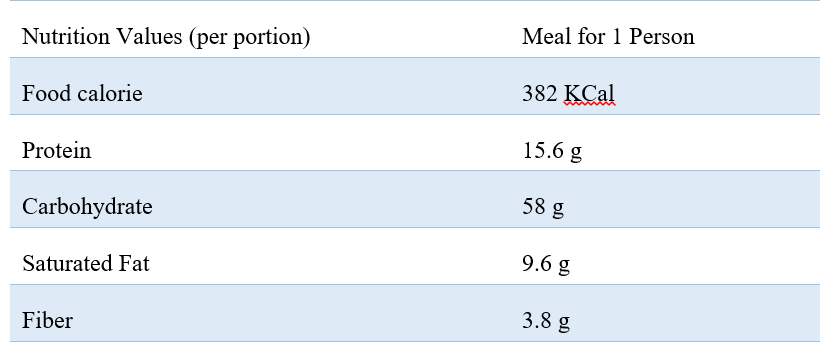
Through learning from long-term patterns of patient behavior, the system can offer a wider range of suitable meals. Based on the example shown in Fig. 2, this particular meal recommendation has its nutrition information listed in Table I.
Table I Nutrition information of recommended meal
The backend sub-system deals with food processing surrounding the services provided by the dietary and meals library, this supports handling and creating of ingredients and recipes. The process entails cook serve, cook freeze, various stages of cook chill, vacuum treatment through to central and satellite kitchen that provides meal delivery services to both individual patients as well as nursing home facilities. One of the advantages is to yield substantial operating cost savings for nursing homes as meals customized for individual clients are delivered in bulk so that the nursing home itself does not need to operate its own cooking facilities. This also saves substantial time and manpower as the meals are specially designed for serving without heating or defrosting upon delivery. Using AI to prepare the meal on demand can ensure freshness and preservation of nutrients, the process is shown in Fig. 3 where automation replaces numerous manual processes that are traditionally required in meal preparation.
These customized dietary solutions are particularly important to patients with stroke, cognitive impairments as well as those undergoing post-surgical rehabilitations. Nutritious soft meals will make a substantial difference to their well-beings [10].

Figure 3 Highly-customized automated meal preparation
In summary, the design and implementation of this AI-based nutrition management system not only provides optimized and customized meals for elderly patients who often have swallow difficulties but also suitable for implantation across the broader smart city environment making the operation of nursing homes more efficient than before. This is particularly important when dealing with the population aging problem that many metropolitan cities currently face. A case study in Japan has shown that by offering soft meals as an alternative to traditional cooking yields a very positive impact on elderly independent living.
References
- Fong, A. C. M., & Usman, M. (2020, December). Machine Thinking for Telehealth–Toward the Next Generation of Healthcare. In 2020 IEEE 2nd International Workshop on System Biology and Biomedical Systems (SBBS) (pp. 1-3).
- McIntosh, M. S. (2011). A clinician’s perspective on incorporating therapeutic lifestyle change into clinical practice. Functional Foods in Health and Disease, 1(2), 50-60.
- Miura, H., Kariyasu, M., Yamasaki, K., & Arai, Y. (2007). Evaluation of chewing and swallowing disorders among frail community‐dwelling elderly individuals. Journal of Oral Rehabilitation, 34(6), 422-427.
- Cocks, T. M., et al. (1999). A protective role for protease-activated receptors in the airways. Nature, 398(6723), 156-160.
- Wu, C. K., et al. (2020). Critical Internet of Things: An interworking solution to improve service reliability. IEEE Communications Magazine, 58(1), 74-79.
- Fong, B., Ansari, N., & Fong, A. C. M. (2012). Prognostics and health management for wireless telemedicine networks. IEEE Wireless Communications, 19(5), 83-89.
- Mohanty, S. P., Choppali, U., & Kougianos, E. (2016). Everything you wanted to know about smart cities: The internet of things is the backbone. IEEE Consumer Electronics Magazine, 5(3), 60-70.
- Wang, T., et al. (2018). Big data reduction for a smart city’s critical infrastructural health monitoring. IEEE Communications Magazine, 56(3), 128-133.
- Fong, B., Fong, A. C. M., & Li, C. K. (2020). Telemedicine Technologies: Information Technologies in Medicine and Digital Health. John Wiley & Sons.
- Yamamoto, T., et al. (2012). Dental status and incident falls among older Japanese: a prospective cohort study. BMJ Open, 2(4).
This article was edited by Bernard Fong
For a downloadable copy of the August 2021 eNewsletter which includes this article, please visit the IEEE Smart Cities Resource Center.


To have the eNewsletter delivered monthly to your inbox, join the IEEE Smart Cities Community.
Past Issues
To view archived articles, and issues, which deliver rich insight into the forces shaping the future of the smart cities. Older eNewsletter can be found here. To download full issues, visit the publications section of the IEEE Smart Cities Resource Center.