Preparation for Natural Disasters in a Smart Nursing Home Environment
Written by T. J. Lu, Ling-Huey Li, Tzu-Wei Chan, Hsin-Yu Lin, and Bernard Fong
Preparation for natural disasters is an extremely important task in the context of emergency and safety management across the smart city framework. This paper takes a look at the preparedness of emergency response in the event of an unpredicted extreme event for smart nursing homes where elderly residents can be endangered by physical and/or cognitive impairments.
Overview
The post-World War II baby boom population has started entering retirement in recent years. With the number of senior citizens increasing steadily over the past decade, there is a growth in demand for nursing homes (Lakdawalla et al., 2013). Nursing homes, also known as convalescent homes, are a type of residential care that provides around-the-clock nursing care for elderly or disabled people. With dementia and psychogeriatric care being widely regarded as residential care, residents of these facilities are particularly vulnerable when dealing with an emergency situation (Fonareva and Oken, 2014). Further, Tängman et al. (2010) suggests that nursing home residents are particularly vulnerable to falls while responding to an emergency situation.
The vulnerability of residents in nursing homes in response to any of the growing list of disasters with a natural or manmade trigger needs to be thoroughly investigated for the safety of residents (Pelling, 2012). Addressing needs when responding to a natural disaster event when assisting elderly residents who may have physical or cognitive impairments is a vitally important aspect of enhancing the safety of senior citizens (Gajos, et al., 2014). This paper, therefore, focuses on investigating the risks associated with a disaster in the nursing home context and studying how staff assist patients with limited mobility to evacuate in the event of an emergency such as flooding, fire, and earthquake. The study also entails the current state of nursing home preparedness to evacuate its patients in the event of a disaster. The research is based on qualitative surveys conducted through interviews with nursing home staff as well as residents to understand possible ways of enhancing the emergency evacuation process in nursing homes.
The results of this research are expected to improve the efficiency of emergency management for senior citizens and specifically benefit the caregivers and management of nursing homes in their new development of emergency response and safety infrastructure for integration into the broader smart city safety and emergency management framework.
Research Objectives
Current methods of disaster response assessment in nursing homes that commonly house a high concentration of senior citizens have fundamental flaws due to their inability to keep pace with an emergency (Kakuma, et. Al., 2013). It is necessary to account for complex mobility profiles, and to address the cognitive decline of residents when handling a disaster (Ngandu, 2015). This is especially problematic given the fact that these nursing homes often have a very high staff-to-resident ratio, the impact on safety, efficiency, and resource management is staggering.
There is a strong need for a major review of disaster response assessment, residents’ state of health, as well as the prediction of the impacts of a disaster on the nursing home staff and patients (Flanagan et al., 2011). There is also a special need to address human factors and environments that affect the way an emergency is managed. The field of human factors was first documented during World War II with the initial aim of enhancing the safety of airplanes (Salvendy, 2012). Human factors focus on a range of different parameters such as ergonomics, safety, human error, and human capability (Bannon, 1995). Human factors apply principles of psychology to minimize safety issues by understanding how people interact with their environments.
Thus, the main purpose of this paper is to derive a radically new approach whose research goals include effective and efficient disaster management for elderly nursing homes that enhances the manual processes by caregivers where human factors play a substantial role in ensuring the safety of patients (Gaba, 2000). The research has collected information about the current status of nursing home preparedness for a disaster and identified several improvement areas, particularly through the introduction of assistive technology. (Finlayson et al., 2016) Therefore, a major change in emergency management assessment is urgently needed (Haddow, 2017), this entails the evaluation of how caregivers cope with an emergency within a very short timeframe and attempt to prepare for an imminent evacuation (Rowland, 2007). There is also a special need to address human factors when ensuring the safety of both patients and their own. A range of personal attributes such as the physical capabilities of the evacuees, psychological factors, and preparedness play a vital role in emergency evacuation (Pan, 2007). In the case of managing an emergency situation that involves staff of different roles, teamwork, communication as well as managing evacuees individually may have a substantial impact on the safety of patients (Leonard, 2004). Most nursing homes have a low staff-to-patient ratio such that it becomes common to apply standard emergency management methods in evacuating their clients in response to a disaster, such that the same plan applies to all situations such as fire, flooding, and earthquake (Bagaria, 2009). Advances in telehealth and assistive technologies have opened up numerous opportunities and possibilities in enhancing various aspects of elderly care (Goodwin, 2010). This research finds that assistive and smart technologies provide numerous opportunities for enhancing the efficiency and effectiveness of emergency management through providing location tracking of all patients as well as providing immediate support and guidance for those in need.
Based on the current understanding of standard textbook methods for emergency management (Waugh, 1999), there are clearly substantial logistical obstacles to interrogating human factors in handling an emergency situation when ensuring the safety of both evacuees and supporting staff. Through the study of current methods for evacuating patients with reduced mobility, an effective, reliable, and credible assistive method and mitigation framework has not yet been developed (Willoughby, et al., 2017). Nursing home clients often have difficulties in responding to an emergency situation (Castle, 2008).
This research envisages enhancing emergency management in a nursing home setting where an individual supporting staff member will be helping many evacuees that require special attention. Informal discussion with nursing home management reveals that a chronic shortage of caregivers often makes one staff member simultaneously support many patients. Some of these elderly patients have individual needs that may require extra help. The results obtained from qualitative analysis are then used for proposing an efficient assistive telehealth-based solution for the efficient management of emergencies (Fong, 2022). This research also studied the human factors associated with emergency response in caregivers in different circumstances, risk modeling, and health economics of mitigation strategies (Dosa, 2008), residents with mobility difficulties may require special assistance during emergency evacuation where there is a strong need for assistive care (Carpenter, 2006).
Problem Statement
Earlier studies have shown traditional emergency handling and disaster prediction methods such as relying on news broadcasts and information from the internet to be significantly flawed, partly as a result of the inability to understand the specific environment of nursing homes and their residents’ health conditions and to account for actual residents’ profiles (Hasegawa et al., 2016). Earlier work concluded that an approach that the inclusion of wireless telemedicine would be necessary to implement assistive care in an efficient manner (Fong, 2013). However, reliance on technology alone is not feasible because of the importance of supporting staff involvement and insufficient knowledge of the specific nature of risks and consequences when a disaster strikes (O'Sullivan et al., 2013)). This is also complicated by the special needs of individual residents and the dependence of aids for the physical conditions of the individual evacuee (Rosenkoetter et al., 2007).
Kholshchevnikov et al. (2012) reported that one major issue associated with emergency evacuation of senior citizens in the event of a fire is mobility concerning the use of crutches since some patients have difficulties with walking on their own, raising the demand for assessing the vulnerability of nursing home residents when dealing with natural hazards (Blaikie et al., 2014). While biomechanical studies have been conducted to address this issue (Carpentier, 2010), various parameters such as cardiopulmonary and postures of the head, trunk spine, and pelvis need to be thoroughly investigated in the event of a sudden evacuation that requires an elderly to rapidly stand up and evacuate in a very short period of time (Hirokawa et al., 2015). The effect of crutch usage on the physiological and functional performance of senior citizens, therefore, needs to be evaluated through gait pattern analysis.
The notion of studying vulnerability regarding elderly residents entails social research methods that take into consideration personal attributes such as mobility, hearing, and recognizing potential hazards that could put certain patients at greater risk when responding to an emergency (Bryman, 2016). Additionally, caregivers may need to carry elderly patients in the event of an emergency evacuation (Cahalan, 2007). These caregivers can be carrying evacuees of close to 100% of their body weight (BW), which far exceeds the safe limits for carrying a load on one’s back (Simpson, et al., 2011), further research should therefore include spine proprioception in load carriage conditions.
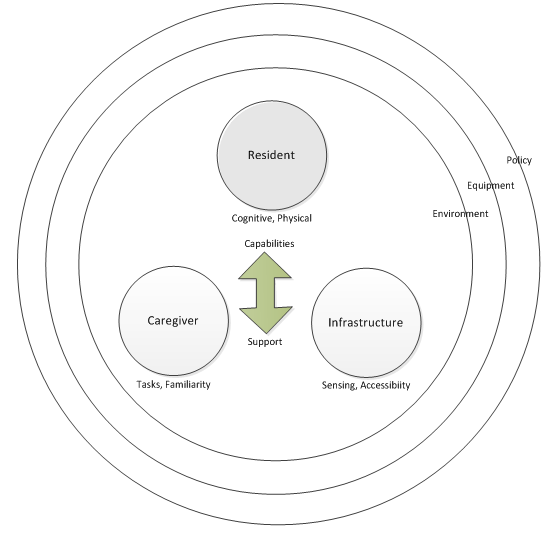
Consumer healthcare devices such as health monitors and smart home gadgets are becoming increasingly popular in recent years. Assistive devices for senior citizens are often made with simplified user interfaces that minimize user interaction. Services currently offered include general monitoring of various health signs and management of chronic diseases through integration with telehealth services. Consumer healthcare technology can help senior citizens that are in need of special attention when responding to disasters such as flooding, fire, and earthquake (Fong et al., 2023). However, one of the most challenging issues to tackle is the usability of such technology given that the end users are either elderly residents or health professionals that may not necessarily have the technical knowledge hence the development of a human-to-machine collaborative environment would be highly desirable as in Fig. 1 (Mahmud, 2022).
Figure 1: Model of human factors of emergency response as part of the smart city infrastructure.
Emergency Management Framework
Qualitative analysis and interviews have been conducted at selected nursing homes to review the current methods of emergency management in response to an unanticipated extreme event. The study involves many complex steps that require various inputs, analysis strategies, and implementation decisions in emergency management. Modeling and drawing inferences from a nursing home requires the extraction of meaningful information from a set of observations as well as interviews with caregivers and residents. As there are practical problems with handling data collected from residents who may suffer from some form of cognitive impairments. Remedial actions such as the automated callouts of telemedicine drones can also be made upon detecting an elderly resident trapped in a hazardous location (Fong et al., 2020). The overall management system is shown in Fig. 2.
Figure 2: Telehealth management system.
Conclusion
Senior citizens are particularly vulnerable to unpredicted extreme events and the utilization of smart technologies in a smart city framework can help prepare elderly residents for a safe and swift evacuation in the event of a natural disaster. Owning to the lack of manpower across many nursing homes the use of such technologies can help enhance the safety and efficiency of emergency management among evacuees that may be suffering from varying degrees of mobility impairments.
References
- Bagaria, J., Heggie, C., Abrahams, J., & Murray, V. (2009). Evacuation and sheltering of hospitals in emergencies: a review of international experience. Prehospital and disaster medicine, 24(5), 461-467.
- Bannon, L. J. (1995). From human factors to human actors: The role of psychology and human-computer interaction studies in system design. In Readings in Human–Computer Interaction (pp. 205-214).
- Blaikie, P., Cannon, T., Davis, I., & Wisner, B. (2014). At risk: natural hazards, people's vulnerability and disasters. Routledge.
- Bryman, A. (2016). Social research methods. Oxford university press.
- Cahalan, C., & Renne, J. (2007). Emergency evacuation of the elderly and disabled. National Emergency Training Center.
- Carpentier, C., Font-Llagunes, J. M., & Kövecses, J. (2010). Dynamics and energetics of impacts in crutch walking. Journal of applied biomechanics, 26(4), 473-483.
- Castle, N. G. (2008). Nursing home evacuation plans. American journal of public health, 98(7), 1235-1240.
- Cutter, S. L., Burton, C. G., & Emrich, C. T. (2010). Disaster resilience indicators for benchmarking baseline conditions. Journal of Homeland Security and Emergency Management, 7(1).
- Do, T. D., Hui, S. C., Fong, A. C. M., & Fong, B. (2009). Associative classification with artificial immune system. IEEE Transactions on Evolutionary Computation, 13(2), 217-228.
- Dosa, D. M., Hyer, K., Brown, L. M., Artenstein, A. W., Polivka-West, L., & Mor, V. (2008). The controversy inherent in managing frail nursing home residents during complex hurricane emergencies. Journal of the American Medical Directors Association, 9(8), 599-604.
- Flanagan, B. E., Gregory, E. W., Hallisey, E. J., Heitgerd, J. L., & Lewis, B. (2011). A social vulnerability index for disaster management. Journal of Homeland Security and Emergency Management, 8(1).
- Finlayson, M., Marrie, R. A., Finlayson, G., Jiang, D., Ekuma, O., Morrow, S., ... & Petrin, J. (2016). Factors Contributing to Nursing Home Entry Among People With Multiple Sclerosis. American Journal of Occupational Therapy, 70(4_Supplement_1), 7011510185p1-7011510185p1.
- Fong, B., Tsang, K. F., & Li, C. K. (2013). Personalized Elderly Assistive Home Care Using 3G Networks. Journal of Advances in Information Technology, 4(3), 136-141.
- Fong, B., Fong, A. C. M., & Tsang, K. F. (2021). Capacity and link budget management for low-altitude telemedicine drone network design and implementation. IEEE Communications Standards Magazine, 5(4), 74-78.
- Fong, B., Kim, H., Fong, A. C. M., Hong, G. Y., & Tsang, K. F. (2022). Self-Cognizant Prognostics for the Design and Implementation of Mission-Critical Telemedicine Systems under the Influence of Heavy Rainfall. IEEE Communications Magazine, 60(8), 80-84.
- Fong, B., Fong, A. C. M., Hong, G. Y., & Tsang, K. F. (2023). Optimization of Power Usage in a Smart Nursing Home Environment. IEEE Transactions on Industry Applications, 59(1), 38-46.
- Fonareva, I., & Oken, B. S. (2014). Physiological and functional consequences of caregiving for relatives with dementia. International Psychogeriatrics, 26(5), 725-747.
- Gaba, D. M. (2000). Anaesthesiology as a model for patient safety in health care. BMJ: British Medical Journal, 320(7237), 785.
- Gajos, A., Kujawski, S., Gajos, M., Chatys, Ż., Bogacki, P., Ciesielska, N., & Zukow, W. (2014). Effect of physical activity on cognitive functions in elderly. Journal of Health Sciences, 4(8), 91-100.
- Gastmans, C., & Milisen, K. (2006). Use of physical restraint in nursing homes: clinical-ethical considerations. Journal of Medical Ethics, 32(3), 148-152.
- Goodwin, N. (2010). The state of telehealth and telecare in the UK: prospects for integrated care. Journal of Integrated Care, 18(6), 3-10.
- Gurses, A. P., Ozok, A. A., & Pronovost, P. J. (2011). Time to accelerate integration of human factors and ergonomics in patient safety. BMJ Qual Saf, bmjqs-2011.
- Haddow, G., Bullock, J., & Coppola, D. P. (2017). Introduction to emergency management. Butterworth-Heinemann.
- Hasegawa, A., Ohira, T., Maeda, M., Yasumura, S., & Tanigawa, K. (2016). Emergency responses and health consequences after the Fukushima accident; evacuation and relocation. Clinical Oncology, 28(4), 237-244.
- Hirokawa, N., Nishiyama, E., Hasegawa, N., Itose, K. I., Shibue, T., Hayami, T., ... & Ohmasa, M. (2015). Study on the safety of a patient who stands up from a chair with a crutch. Procedia Manufacturing, 3, 74-81.
- Kakuma, R., Fort, D., Galbaud, G., Arsenault, L., Perrault, A., Platt, R. W., ... & Wolfson, C. (2003). Delirium in older emergency department patients discharged home: effect on survival. Journal of the American Geriatrics Society, 51(4), 443-450.
- Karsh, B. T., Holden, R. J., Alper, S. J., & Or, C. K. L. (2006). A human factors engineering paradigm for patient safety: designing to support the performance of the healthcare professional. BMJ Quality & Safety, 15(suppl 1), i59-i65.
- Kholshchevnikov, V. V., Samoshin, D., & Istratov, R. (2012). The problems of elderly people safe evacuation from senior citizen heath care buildings in case of fire. In Proceedings of 5th International Symposium" Human Behaviour In Fire". Cambridge. UK (pp. 587-593).
- Lakdawalla, D., Goldman, D. P., Bhattacharya, J., Hurd, M. D., Joyce, G. F., & Panis, C. W. (2003). Forecasting the nursing home population. Medical Care, 41(1), 8-20.
- Leonard, M., Graham, S., & Bonacum, D. (2004). The human factor: the critical importance of effective teamwork and communication in providing safe care. BMJ Quality & Safety, 13(suppl 1), i85-i90.
- Mahmud, B. U., (2022). A Study of Human-AI Symbiosis for Creative Work: Recent Developments and Future Directions in Deep Learning. ACM Transactions on Multimidia Computing Communications and Applications.
- Ngandu, T., Lehtisalo, J., Solomon, A., Levälahti, E., Ahtiluoto, S., Antikainen, R., ... & Lindström, J. (2015). A 2 year multidomain intervention of diet, exercise, cognitive training, and vascular risk monitoring versus control to prevent cognitive decline in at-risk elderly people (FINGER): a randomised controlled trial. The Lancet, 385(9984), 2255-2263.
- O'Sullivan, T. L., Kuziemsky, C. E., Toal-Sullivan, D., & Corneil, W. (2013). Unraveling the complexities of disaster management: A framework for critical social infrastructure to promote population health and resilience. Social Science & Medicine, 93, 238-246.
- Pan, X., Han, C. S., Dauber, K., & Law, K. H. (2007). A multi-agent based framework for the simulation of human and social behaviors during emergency evacuations. Ai & Society, 22(2), 113-132.
- Pelling, M. (2012). The vulnerability of cities: natural disasters and social resilience. Routledge.
- Rosenkoetter, M. M., Covan, E. K., Cobb, B. K., Bunting, S., & Weinrich, M. (2007). Perceptions of older adults regarding evacuation in the event of a natural disaster. Public Health Nursing, 24(2), 160-168.
- Rowland, J. L., White, G. W., Fox, M. H., & Rooney, C. (2007). Emergency response training practices for people with disabilities: Analysis of some current practices and recommendations for future training programs. Journal of Disability Policy Studies, 17(4), 216-222.
- Salvendy, G. (2012). Handbook of human factors and ergonomics. John Wiley & Sons.
- Simpson, K. M., Munro, B. J., & Steele, J. R. (2011). Backpack load affects lower limb muscle activity patterns of female hikers during prolonged load carriage. Journal of Electromyography and Kinesiology, 21(5), 782-788.
- Tängman, S., Eriksson, S., Gustafson, Y., & Lundin-Olsson, L. (2010). Precipitating factors for falls among patients with dementia on a psychogeriatric ward. International psychogeriatrics, 22(4), 641-649.
- Willoughby, M., Kipsaina, C., Ferrah, N., Blau, S., Bugeja, L., Ranson, D., & Ibrahim, J. E. (2017). Mortality in nursing homes following emergency evacuation: a systematic review. Journal of the American Medical Directors Association, 18(8), 664-670.
- Waugh, W. L. (1999). Living with hazards, dealing with disasters: An introduction to emergency management. ME Sharpe.
This article was edited by Melkior Ornik.
To view all articles in this issue, please go to April 2023 eNewsletter. For a downloadable copy, please visit the IEEE Smart Cities Resource Center.





To have the eNewsletter delivered monthly to your inbox, join the IEEE Smart Cities Community.
Past Issues
To view archived articles, and issues, which deliver rich insight into the forces shaping the future of the smart cities. Older eNewsletter can be found here. To download full issues, visit the publications section of the IEEE Smart Cities Resource Center.